Your Cart
Your Cart is currently empty.
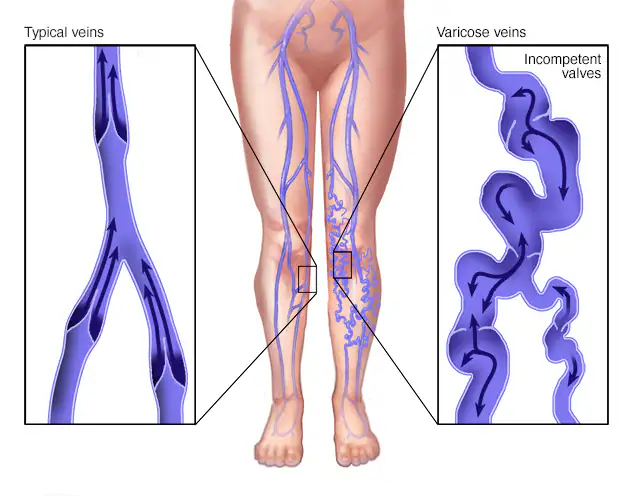
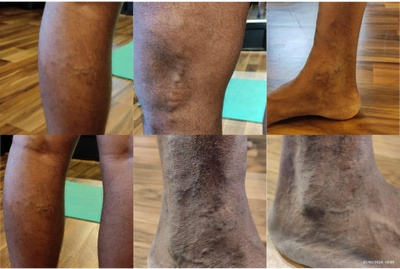
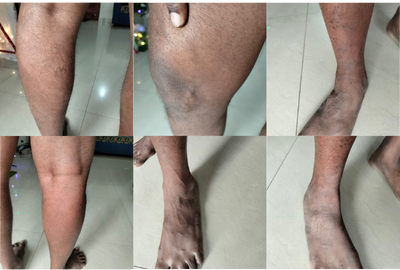
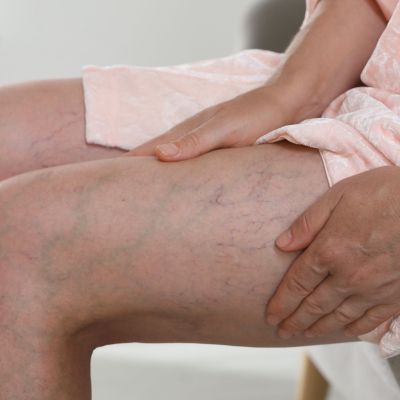
Varicose veins are enlarged, twisted veins, most commonly in the legs, caused by malfunctioning valves that allow blood to pool and veins to enlarge. Spider veins are a minor form of varicose veins. Varicose veins are often hereditary and can worsen with age, standing for long periods, or poor liver function.
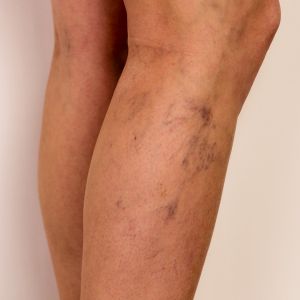
Swollen, twisted veins

Leg pain or aching
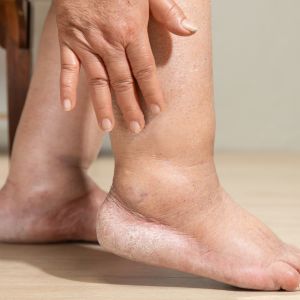
Swelling in the ankles and lower legs
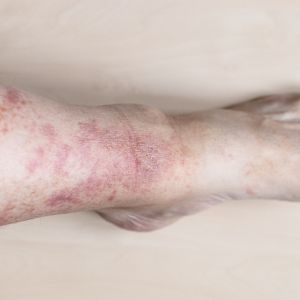
Itchy or irritated skin

Muscle cramps or restless legs
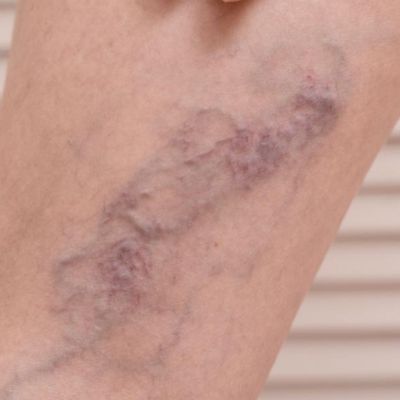
Varicose veins increase the risk of surface vein clots and, rarely, deep vein thrombosis, which can lead to pulmonary embolism.
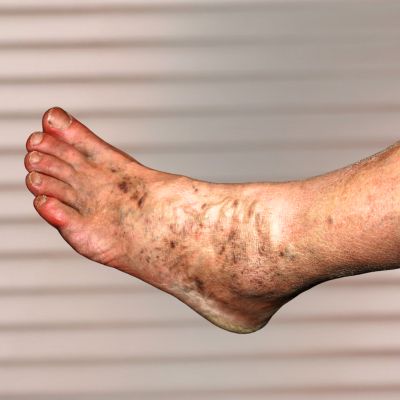
Prolonged venous pressure can impair blood flow back to the heart, causing skin changes, swelling, and ulcerations.
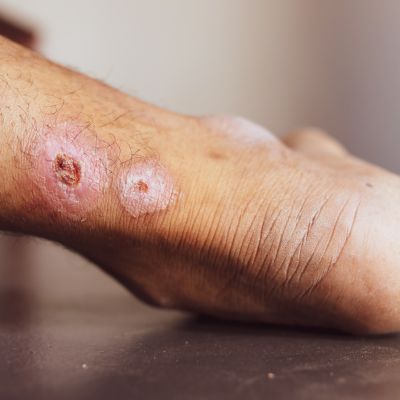
Untreated varicose veins can cause venous ulcers near the ankles, with a 3–5% higher risk over time.
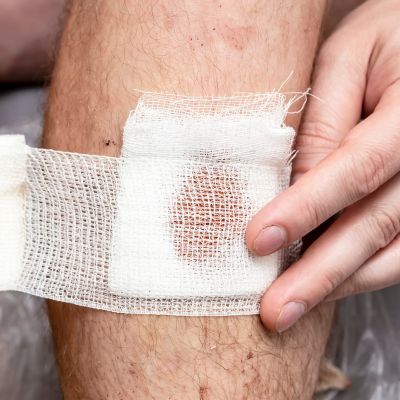
Varicose veins close to the skin’s surface are at risk of rupturing, causing unexpected and sometimes severe bleeding.
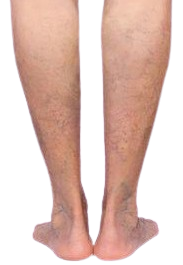
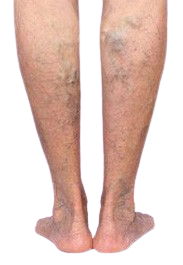
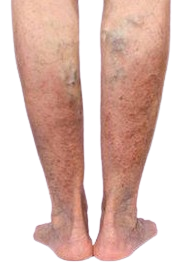
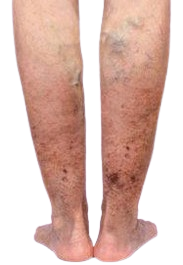
The existing treatment available to cure varicose veins is the predominant usage of anti-coagulant, which has its own set of side-effects. The limitations with blood-thinners are that it doesn’t address the root cause i.e. liver abnormalities. Adding on, the blood thinning agents cause severe bleeding in any part of the body in the long term. The long-term usage of blood thinners can also result in blood in urine / stool and can lead to heavier menstrual flows.
Phone number:
+91 6379926961
Location:
429A, V.V.C Layout, Pulliyakulam Road, Coimbatore – 641018.
Email:
support@namashivayah.com